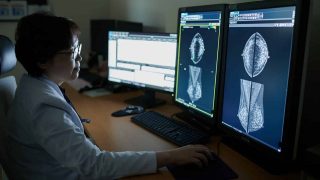
‘Smart bandages’ combining biological monitoring and wound treatment have been tested for years – but with a new type of bandage based on nanomaterials, a team of RMIT University scientists have made them cost-effective as well.
The School of Engineering researchers have developed a hydrogel dressing embedded with miniscule nanomaterials, also known as carbon dots, that sense changes in a wound such as the rise in pH that is a telltale sign of a local infection.
Embedded carbon dots change colour when such a change is detected, providing a map of developing infections that can be read by portable sensors, to help doctors adjust wound management to speed healing.
The smart bandages are also impregnated with therapeutic ‘nanozymes’ – synthetic enzymes designed to perform a specific function – that can be released to promote healing of the wound, either automatically or by rubbing on the bandage to release them.
“Being able to address potential infection at the earliest opportunity is critical to chronic wound management, making this real-time system a potential gamechanger for healthcare,” said study lead Nan Nan, an RMIT PhD candidate.
Fabrication of the new smart bandages “is easy and scalable,” she said, “with strong potential for commercial translation.”
Early smart bandages are promising but complex
Wound care is fundamental to healthcare, but commercial translation is critical to make products cost-effective enough for use in large quantities – yet many systems have been so heavily engineered that they’re impractical or too expensive for widespread use.
One early prototype highlighted those complexities, with an entire microchip linked to an array of sensors made possible by the rise of flexible electronics that can be bent to follow the shape of the skin.
While technically promising, the design was complex and expensive.

RMIT University's Dr Lei Bao, Nan Nan, and Dr Haiyan Li. Image: RMIT University / Supplied
In 2022, a National University of Singapore team built a complex bandage with sensors that detect and classify bacteria and inflammatory factors, as well as measuring acidity and temperature, in a 15 minute test that transmits results to a mobile app.
Last year, Caltech researchers devised a way to continually monitor wound fluids, while a University of Nebraska team demonstrated an ‘electroceutical’ bandage combining a nerve-repair drug with electrical pulses that speed wound closure and boost skin regeneration.
And Saudi Arabian researchers built a smart bandage that used electric fields and embedded electrodes to deliver electric current that “significantly enhance[d] wound healing” in lab rats – with a machine learning (ML) model trained on vital signs as the wound healed.
The path to commercialisation
ML is another frontier in smart bandages: if algorithms can be trained to spot the signs of infection given off by biomarkers embedded in bandages, doctors can use them to better monitor a wound’s progress and adjust management to speed healing.
One recent US study found an AI-powered wearable device called a-Heal could speed wound healing by around 25 per cent compared with standard care, using a camera to track wound progress and bioelectronics to accelerate healing.
Such advances hold great promise not only for commodity bandages you might have in the medicine cabinet for cuts and scrapes, but for management of chronic ulcers, pressure sores, and other injuries that incur $3.5 billion in healthcare costs per year in Australia alone.
Yet the laboratory is a long way from the hospitals and homes where smart bandages could do the most good – and even if the science shows promise, commercialising the bandages requires scaling their manufacturing and integrating them into healthcare supply chains.
Scalability is key for a separate team of RMIT University researchers that last year demonstrated a microchip-based wound monitoring wearable with sensors that track inflammation, pH, and temperature changes.
Lead inventor Dr Peter Elango said the device could be mass-produced for less than $5 per unit at scale, with the team currently canvassing industry and manufacturing partners to make it happen.
Another smart bandage team believes its device would cost in the “tens of dollars” for a patch that can be used for one to two weeks – expensive for everyday use on small cuts, but far more reasonable in simplifying the complex management of chronic wounds.
RMIT University senior lecturer Dr Haiyan Li believes the simplicity of Nan’s hydrogel-based approach could be a breakthrough for commercialising smart bandages after years of translation challenges.
“Many smart wound dressings developed in research labs are difficult to translate into real clinical products because they rely on complex designs or expensive sensing systems,” she said, noting Nan’s work “has defined concise design rules for future smart dressings.”
“Our approach integrates sensing and dual-mode therapeutic functions into a single dressing with a simple, streamlined design, which helps address some of the key challenges that have previously limited commercial translation.”